Nervous system regulation is not chakras. It is not crystal energy. It is not manifestation. It is the application of established neuroscience principles to restore a dysregulated autonomic nervous system to functional regulation. It is measurable, reproducible, and backed by decades of peer-reviewed research.
Nervous system regulation is clear: this is not wellness conjecture. It is peer-reviewed neuroscience, measurable physiology, and reproducible clinical outcomes. The wellness space is saturated with vague claims, untraceable credentials, and practitioners who substitute language for mechanism. You’re right to demand more.
I’m an engineer by background. I don’t work from intuition. I work from mechanism. And when I first encountered clinical nervous system regulation, I applied the same scrutiny you’re applying now. What changed my position wasn’t a testimonial or a feeling. It was data: peer-reviewed research, measurable physiological markers, and my own post-stroke reconstruction — measured by my medical team at every stage.
Nervous system regulation is not chakras. It is not crystal energy. It is not manifestation. It is the application of established neuroscience principles to restore a dysregulated autonomic nervous system to functional regulation. It is measurable, reproducible, and backed by decades of peer-reviewed research.
This article lays out the mechanism, the evidence, and the clinical approach — so you can evaluate it on its merits.
What Nervous System Recovery Actually Is
Your autonomic nervous system (ANS) regulates every involuntary function in your body: heart rate, respiratory rhythm, digestion, immune response, inflammation levels, hormonal cycles. It operates through two primary branches — the sympathetic system (activation, threat response) and the parasympathetic system (recovery, rest, regeneration) — mediated largely by the vagus nerve. For a clinical breakdown of burnout specifically, see Nervous System Recovery From Burnout.
When this system is regulated, you shift fluidly between activation and recovery. When it is dysregulated — as happens with chronic stress, burnout, or trauma — your nervous system gets stuck in a threat-detection state. It loses the capacity to return to baseline. This is not a metaphor. It is a measurable physiological condition.
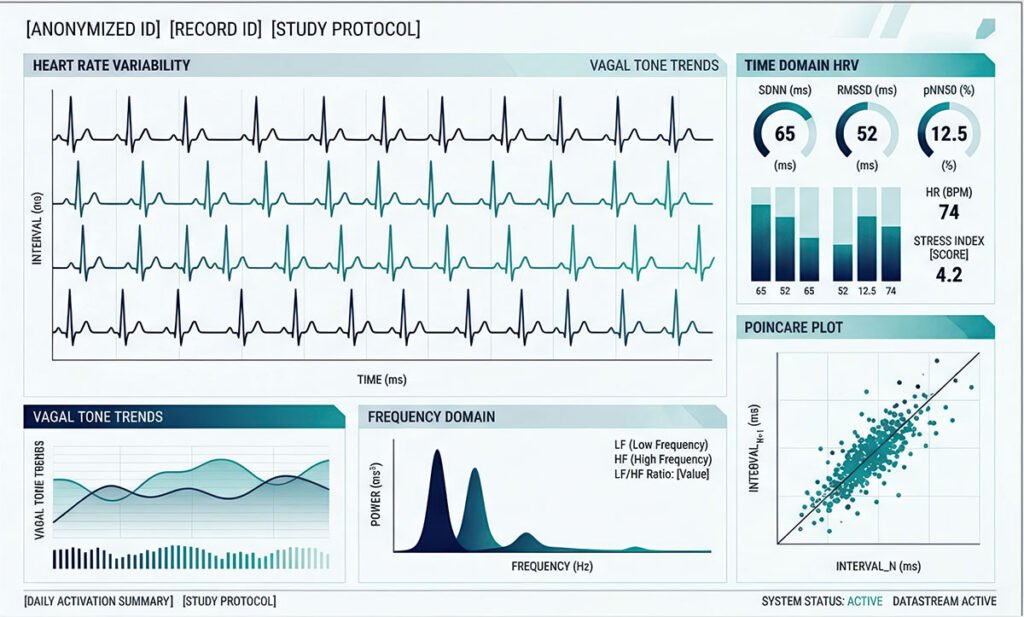
The primary metric for nervous system regulation is Heart Rate Variability (HRV). HRV measures the variation in time intervals between heartbeats — a direct indicator of vagal tone, which is the functional capacity of your vagus nerve. High HRV correlates with robust vagal tone, effective stress recovery, and resilient health. Low HRV correlates with chronic stress, inflammation, immune dysfunction, and nervous system dysregulation. This is established science, validated across thousands of studies and recognized by the European Society of Cardiology and the North American Society of Pacing and Electrophysiology (Task Force, 1996).
Nervous system recovery, then, is the process of restoring vagal tone and autonomic regulation through targeted physiological intervention. It does not require belief. It requires stimulus, mechanism, and measurement.
How This Differs From Therapy, Meditation, and Medication
Talk therapy operates primarily through the prefrontal cortex — the thinking, reasoning brain. It can reshape cognitive patterns over time, but it does not directly stimulate the autonomic nervous system. This is why therapy is valuable for psychological insight but often slow to produce measurable nervous system change.
Meditation builds vagal tone awareness gradually, but requires sustained daily practice and struggles to penetrate severe dysregulation. If your nervous system is locked in threat mode, asking it to “relax” through meditation is asking the cortex to override the brainstem — a mismatch in neurological authority.
Medication (anxiolytics, SSRIs, sleep aids) manages symptoms downstream of the dysregulation without addressing the dysregulation itself. It suppresses output without correcting the autonomic input.
Clinical nervous system recovery works at the autonomic level directly. It targets the vagus nerve and the ventral vagal pathway, bypassing the cortex entirely. This is why measurable changes — HRV improvement, sleep normalization, anxiety reduction — appear faster than with cortex-mediated approaches.
The Mechanism: How Nervous System Recovery Works
The foundational framework is Polyvagal Theory, developed by neuroscientist Stephen Porges (2011). Polyvagal Theory identifies three distinct neural circuits within the vagal system, each corresponding to a different physiological state:
- Ventral Vagal Complex (newest evolutionarily) — governs safe social engagement, calm alertness, and recovery. This is the state your nervous system needs to reach for genuine regulation.
- Sympathetic Nervous System — governs mobilization: fight-or-flight responses, action under threat, adrenaline-mediated activation.
- Dorsal Vagal Complex (oldest evolutionarily) — governs immobilization: freeze, shutdown, dissociation. This is the state that chronic burnout often produces.
In a regulated nervous system, you can move fluidly between these states depending on context. In a dysregulated nervous system, this fluidity breaks down. Most burnout clients are stuck in either chronic sympathetic activation (hypervigilance, anxiety, insomnia, racing thoughts) or dorsal vagal collapse (exhaustion, dissociation, numbness) — or they oscillate unpredictably between both.
How Clinical Recovery Restores Regulation
Clinical nervous system recovery works by directly stimulating the ventral vagal pathway. When this pathway activates, several measurable things happen simultaneously:
- Heart rate variability increases (measurable via HRV monitoring)
- Heart rate pattern becomes more coherent
- Respiratory sinus arrhythmia normalizes
- Cortisol and inflammatory markers trend downward
- Sleep architecture begins to restore — deeper REM cycles, fewer awakenings
These are physiological events, measurable in real time or within days of intervention. Your nervous system does not need to “believe” in the process. It registers the vagal stimulus physiologically, regardless of your cognitive expectations.
My Clinical Approach
Why an Engineering Background Matters
I approach nervous system recovery as an engineering problem. I measure inputs (your current nervous system state — sleep patterns, energy levels, anxiety markers, HRV if available). I apply a specific intervention (clinical protocol based on polyvagal theory and vagal stimulation). I measure outputs (changes in sleep, energy, anxiety, HRV). If the outputs don’t change, the protocol changes. No spiritualism. No faith required. Just applied neuroscience with a feedback loop.
Proof of Concept: Post-Stroke Nervous System Reconstruction
At 57, I suffered a stroke. My vagal dysregulation was severe and confirmed by medical testing. My HRV dropped to 22 — well below the threshold for healthy functioning. Sleep was destroyed. My nervous system was locked in chronic threat-detection mode. Conventional rehabilitation addressed motor recovery but did not target the autonomic dysregulation.
I applied clinical nervous system recovery protocols to my own reconstruction — protocols grounded in polyvagal theory, vagal stimulation, and neuroplasticity research. My HRV improved measurably within 4 weeks. Within 12 weeks, it reached 65 (healthy range). These numbers were tracked by my medical team. This was not placebo. It was not spontaneous remission. It was a targeted intervention producing a measurable, reproducible result.
Ready to start your recovery?
Check If You QualifyWhat Happens in a 50-Minute Session

- Assessment and explanation.
Before any intervention, I evaluate your current nervous system state and explain what I’m observing. You understand the mechanism before we begin. - Clinical vagal stimulation.
I work with your nervous system using a specific protocol designed to activate the ventral vagal pathway. You may experience warmth, tingling, deep physical relaxation, or no obvious sensation during the session itself. - Nervous system re-education.
I explain what happened physiologically, so your nervous system learns to recognize and sustain the regulated state. - Measurement.
You track sleep quality, energy level, and anxiety on a simple scale between sessions. If you use an HRV-capable device, we track HRV trends over time. You always know whether recovery is progressing.
How This Differs From Other Practitioners
If you’ve tried other practitioners in this space and left disappointed, your skepticism was earned. Here is what typically goes wrong, and why my approach is structurally different.
The Problem With Intuition-Based Practice
Many practitioners operate from intuition. They use language like “raising your vibration,” “unblocking energy,” or “realigning your field.” These terms are evocative but unmeasurable. There is no way to determine whether anything actually changed in your nervous system. No baseline. No metric. No reproducibility.
What a Clinical Approach Looks Like
A clinical approach to nervous system recovery has three non-negotiable characteristics:
- Defined mechanism — the practitioner can explain exactly what is happening physiologically and cite the research that supports it.
- Measurable outcomes — you track objective markers (sleep quality, HRV, energy, anxiety) before, during, and after the intervention.
- Transparency — the practitioner explains what they’re doing and why at every stage. If you ask “what just happened?” you get a physiological answer, not a metaphysical one.
What Clients Say
The following testimonials were collected during an earlier phase of my practice. The modality has evolved — the results have not.

“I had been dealing with a chronic physical condition for years — six years of conventional treatment that provided a band-aid at best. My session with Vincent was scheduled for 30 minutes. Within minutes, I felt a release throughout my entire body. The symptoms cleared. Weeks later — still clear.”
— Nancy Squier, Scottsdale, AZ, USA

“I felt quite lost, stuck, and in pain. After working with Vincent, I now feel centred, calm, and functional in a way I hadn’t for a long time. The recovery was faster than I expected.”
— Valerie Brockbank, Los Angeles, USA
The Research Behind This Approach
Polyvagal Theory
Porges’ Polyvagal Theory (2011) establishes that the vagus nerve operates through three hierarchical circuits — ventral vagal, sympathetic, and dorsal vagal — each governing a distinct physiological state. The ventral vagal complex is the target of clinical nervous system recovery.
Porges, S. W. (2011). The Polyvagal Theory. W. W. Norton & Company.
Heart Rate Variability as a Health Marker
HRV is the gold standard for measuring autonomic nervous system regulation. Higher HRV indicates better parasympathetic function; lower HRV indicates dysregulation. This metric is used across cardiology, psychiatry, sports science, and clinical practice.
Task Force of the European Society of Cardiology. (1996). Circulation, 93(5), 1043–1065.
Vagal Tone and Inflammation
Tracey’s research demonstrates that vagal tone directly modulates the inflammatory reflex. Improving vagal tone doesn’t just reduce anxiety — it lowers measurable inflammatory markers throughout the body.
Tracey, K. J. (2009). Nature Reviews Immunology, 9(6), 418–428.
Neuroplasticity
The nervous system’s capacity to rewire itself is the scientific foundation for all nervous system recovery. Targeted, repeated stimulation creates lasting structural and functional changes in neural pathways.
Merzenich, M. M. et al. (2014). Frontiers in Human Neuroscience, 8, 385.
Vagal Tone and Emotional Regulation
Kemp and Quintana’s review consolidates evidence that resting-state HRV is a biomarker for emotional regulation capacity. Higher vagal tone correlates with better stress recovery and lower vulnerability to anxiety and depression.
Kemp, A. H., & Quintana, D. S. (2013). International Journal of Psychophysiology, 89(3), 288–296.
Frequently Asked Questions
Is there actually peer-reviewed research supporting this?
Yes. The research base includes polyvagal theory (Porges), HRV studies (Task Force, 1996), vagal-immune interaction research (Tracey, 2009), and neuroplasticity research (Merzenich et al.). Search “polyvagal theory” or “vagal tone” on PubMed and you’ll find hundreds of peer-reviewed publications. This is not fringe science. It is established neuroscience with clinical applications.
How do I know if recovery is actually working?
You measure it. Before sessions begin, we establish a baseline: sleep quality, energy level, anxiety level, and HRV if you have a wearable device. After each session, you track the same metrics. Most clients see measurable improvement within 4 weeks. If you are not seeing improvement, the protocol is adjusted. There is no ambiguity and no reliance on subjective feeling alone.
Is this a substitute for medical treatment?
No. If you have a diagnosed medical condition, continue working with your doctor. Clinical nervous system recovery is complementary — it targets autonomic dysregulation in ways that conventional treatment often does not address directly. But it is not a replacement for medical care.
Why haven’t I heard of this approach before?
Because most practitioners in this space don’t use clinical language, don’t cite research, and don’t measure outcomes. When you apply rigor — defined mechanism, peer-reviewed research, measurable results — nervous system recovery becomes a legitimate clinical discipline. The evidence has been there for decades. The clinical application is what’s catching up.
How is this different from vagus nerve stimulation devices?
Vagus nerve stimulation (VNS) devices deliver electrical impulses to the vagus nerve. Clinical nervous system recovery uses a different modality — working with the body’s own regulatory mechanisms through targeted clinical protocols rather than electrical stimulation. Both target the vagus nerve. The measurable outcomes — HRV improvement, sleep normalization, reduced anxiety — are comparable.
The Science Is Clear
Your nervous system can recover through clinical approaches backed by peer-reviewed research. The mechanism is defined. The outcomes are measurable.